NOTA for $199 + unlim scan forever!
Weekend promotion! 35% discount on the Unlimited package.
Valid until January 31, 2023
Valid until January 31, 2023
Days
Hours
Minutes
Seconds
Subungual(nail) melanoma: symptoms, stages, photos
Subungual melanoma is a type of skin cancer that occurs under the nails. It is a rare form of melanoma that develops unrelated to sun exposure.
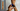
Many people who find a spot under their fingernail begin to search the Internet (or send photos to Reddit), what could it be? And it turns out that this may be a fatal disease - subungual or nail melanoma.
Subungual melanoma is a type of skin cancer that occurs under the nails. It is a rare form of melanoma that develops unrelated to sun exposure. Of the total number of melanomas, the proportion of this tumor is only 2% [1, 2, 3]. The indicator is quite low, but this does not negate the possibility of getting sick.
For representatives of other skin phototypes other than the 2nd, the chances may vary greatly. Representatives of the Mongoloid and Negroid races have a higher (up to 40%) chance of getting melanoma of the nail bed [4, 5].
Subungual melanoma is a type of skin cancer that occurs under the nails. It is a rare form of melanoma that develops unrelated to sun exposure. Of the total number of melanomas, the proportion of this tumor is only 2% [1, 2, 3]. The indicator is quite low, but this does not negate the possibility of getting sick.
For representatives of other skin phototypes other than the 2nd, the chances may vary greatly. Representatives of the Mongoloid and Negroid races have a higher (up to 40%) chance of getting melanoma of the nail bed [4, 5].
"
Where does nail melanoma appear more often? The tumor affects the big toes more often[3].
What does a subungual melanoma look like? Photos and signs.
All the pictures below have histological confirmation, and are not taken from the Internet. The source is indicated in square brackets. There are 2 most common signs:
Feature I
Most often, nail melanoma manifests itself in the form of a strip of brown or black color. The strip starts from the nail roller and ends at the edge of the nail. This condition is called longitudinal melanonychia. Some medications can lead to the appearance of such bands – retinoids and Docetaxel (Taxotere) [10]. This sign can also be in conditions unrelated to melanoma, for example, with a fungal lesion of the nail, a pigmented nevus of the nail bed.
All the pictures below have histological confirmation, and are not taken from the Internet. The source is indicated in square brackets. There are 2 most common signs:
Feature I
Most often, nail melanoma manifests itself in the form of a strip of brown or black color. The strip starts from the nail roller and ends at the edge of the nail. This condition is called longitudinal melanonychia. Some medications can lead to the appearance of such bands – retinoids and Docetaxel (Taxotere) [10]. This sign can also be in conditions unrelated to melanoma, for example, with a fungal lesion of the nail, a pigmented nevus of the nail bed.
Feature II
The most common sign of this type of melanoma is Hutchinson's symptom - the transition of pigmentation to the nail roller or finger tip. In 7 of the 8 images presented below, this feature is visible. At the same time, it cannot be unequivocally stated that this symptom occurs only with melanoma. It can also be observed with a transparent cuticle [10].
The most common sign of this type of melanoma is Hutchinson's symptom - the transition of pigmentation to the nail roller or finger tip. In 7 of the 8 images presented below, this feature is visible. At the same time, it cannot be unequivocally stated that this symptom occurs only with melanoma. It can also be observed with a transparent cuticle [10].

Subcutaneous pigmented nevus in a 13-year-old boy [9]

Subungual melanoma of the I st., 0.2 mm according to Breslow [10]

8 cases of subungual melanoma in situ (initial stage) [6]
Promptly! Regularly! At home!
Buy your personal mole tracker and monitor your skin health right in the comfort of your home!
The set includes: NOTA mole tracker, 2 scan heads, 2 velvet storage bag, 20 alcohol wipes, USB cable.


3 trial months in the app.
- $5/month after the end of the trial;
- Unlimited number of measurements;
- Suitable for the whole family;
- Buy for 4 interest-free payments;
- Delivery - $20.
No subscriptions forever!
- Free use of the app;
- Unlimited number of measurements;
- Suitable for the whole family;
- Buy for 4 interest-free payments;
- Free delivery.
NOTA + subscription for $199
NOTA unlimited for $320


How to distinguish subungual melanoma from everything else?
Here is a fairly simple algorithm:
- Age ≥ 50 years.
- Race: Mongoloid, Americanoid, Negroid.
- Stripes ≥ 3 mm, black, with fuzzy edges, occupy more than ⅔ of the nail plate.
- The thumb of the hand or foot, the index finger of the affected or dominant hand.
- The transition of pigmentation to the nail roller, the tip of the finger (Hutchinson's symptom) or the free edge of the nail.
- Melanoma or dysplastic nevus syndrome in the patient or relatives in the past.
- Destruction or dystrophy of the nail.
- According to the results of dermatoscopy, irregular stripes are uneven in thickness or color.
- Age ≥ 50 years.
- Race: Caucasian, Latin American
- Stripe ≤ 3 mm brown, clearly defined, occupy less than ⅓ of the nail plate.
- Remains unchanged for months or years.
- Fingers 3-5 or toes 2-5 of the affected or non-dominant hand.
- There is no pigmentation on the nail roller, fingertip or free edge of the nail.
- The patient and his relatives do not have and have not had melanoma and dysplastic nevus syndrome in the past.
- There is no destruction or dystrophy of the nail.
- According to the results of dermatoscopy, regular stripes are uniform in thickness and color.




Single
Multiple
Are the stripes the same in color and width?
Monitoring
Monitoring
Contact an oncologist for a biopsy
NO
YES
Longitudinal melanonychia
- A (age) age - the peak incidence of subungual melanoma occurs at the age of 50 to 70 years, and also indicates races with increased risk: Asians, Africans - they account for 1/3 of all cases of melanoma.
- B (brown to black) – the color is brown and black, with a band width of more than 3 mm and vague borders.
- C (change) – a change in the color of the nail plate or the absence of changes after treatment.
- D (digit) - the finger as the most frequent place of injury.
- E (extension) - the spread of pigmentation on the nail roller or finger tip (Hutchinson's symptom).
- F (Family) - relatives or the patient has melanoma in the past or dysplastic nevus syndrome. [11]
"
"
Scheme: What can be on our nail.
How to distinguish subarticular melanoma from everything else? Here is a fairly simple algorithm.
Conclusion:
Subungual (nail-bed)melanoma is a tumor that is difficult enough for early diagnosis. The most common signs are the presence of a stripe on the nail and the transition of pigmentation to the nail roller or finger tip. If you find yourself with one of these symptoms, you need to see an oncologist.
P.S.: If you happen to be at a dermatologist or oncologist's appointment, show him your nails. If you apply nail polish, it is better to remove it before taking it.
Subungual (nail-bed)melanoma is a tumor that is difficult enough for early diagnosis. The most common signs are the presence of a stripe on the nail and the transition of pigmentation to the nail roller or finger tip. If you find yourself with one of these symptoms, you need to see an oncologist.
P.S.: If you happen to be at a dermatologist or oncologist's appointment, show him your nails. If you apply nail polish, it is better to remove it before taking it.
The ABCDEF rule in the diagnosis of melanoma of the nail bed.



List of literature
- Miller AJ, Mihm MC. Melanoma. N Engl J Med.; 355:51-65.
- Data from the Globocan 2019 study by the International Agency for Research on Cancer (IARC)
- Kuchelmeister C, Schaumburg-Lever G, Garbe C. Acral cutaneous melanoma in caucasians: clinical features, histopathology and prognosis in 112 patients // J. Dermatol.
- Takematsu H, Obata M, Tomita Y. Subungual melanoma. A clinicopathologic study of 16 Japanese cases // Cancer.
- Wu XC, Eide MJ, King J. Racial and ethnic variations in incidence and survival of cutaneous melanoma in the United States, 1999–2006 // J. Am. Acad. Dermatol.
- Jae Ho Lee, Ji-Hye Park, Jong Hee Lee, Dong-Youn Lee. Early Detection of Subungual Melanoma In Situ: Proposal of ABCD Strategy in Clinical Practice Based on Case Series Ann Dermatol; 30(1): 36–40.
- Stephan Braun, MD and Peter Gerber, MD. Subungual malignant melanoma. CMAJ. 187(12): 909.
- Pierre Halteh, Richard Scher, MD, FACP, Amanda Artis, MS, MPH, and Shari R. Lipner, MD, PhD. A Survey Based Study of Management of Longitudinal Melanonychia Amongst Attending and Resident Dermatologists. J Am Acad Dermatol.; 76(5): 994–996.
- Kamran Khan and Arun A Mavanur. Longitudinal melanonychia. BMJ Case Rep.: bcr2015213459.
- Holger A. Haenssle, Andreas Blum, Rainer Hofmann-Wellenhof, Juergen Kreusch, Wilhelm Stolz, Giuseppe Argenziano, Iris Zalaudek, and Franziska Brehmer. When all you have is a dermatoscope— start looking at the nails. Dermatol Pract Concept.; 4(4): 11–20.
- Levit EK, Kagen MH, Scher RK, Grossman M, Altman E. The ABC rule for clinical detection of subungual melanoma. J Am Acad Dermatol. ;42(2 Pt 1):269-74.
- Haenssle HA, Brehmer F, Zalaudek I, Hofmann-Wellenhof R, Kreusch J, Stolz W, Argenziano G, Blum A. Dermoscopy of nails. Hautarzt.;65(4):301-11. doi: 10.1007/s00105-013-2707-x.



