Nodular melanoma: photos, symptoms, treatment
In this article we will tell and show what nodular melanoma looks like and how to treat it.

For nodular melanoma, the extended ABCDE rule is used, to which the letters EFG are added.
E - Elevated. Benign lesions can be elevated (e g, a dermal naevus, dermatofibroma, or cyst), but a new elevated or thickened lesion may be suspicious for nodular melanoma or another form of skin cancer.
F - Firm. Benign lesions can feel firm (especially dermatofibroma), but this is also a feature of nodular melanoma.
G - Growing. A nodular melanoma tends to grow rapidly with changes noted over days or weeks. Benign skin lesions tend to remain stable or change slowly over years to decades. Although they can rapidly change in appearance over hours to days if injured, inflamed, bleeding, or affected by eczema, they do not usually grow in size.
It is also worth noting that the malignant formation often loses its characteristic skin pattern, becomes smooth and shiny.
E - Elevated. Benign lesions can be elevated (e g, a dermal naevus, dermatofibroma, or cyst), but a new elevated or thickened lesion may be suspicious for nodular melanoma or another form of skin cancer.
F - Firm. Benign lesions can feel firm (especially dermatofibroma), but this is also a feature of nodular melanoma.
G - Growing. A nodular melanoma tends to grow rapidly with changes noted over days or weeks. Benign skin lesions tend to remain stable or change slowly over years to decades. Although they can rapidly change in appearance over hours to days if injured, inflamed, bleeding, or affected by eczema, they do not usually grow in size.
It is also worth noting that the malignant formation often loses its characteristic skin pattern, becomes smooth and shiny.
In nodular melanoma, melanoma cells proliferate downwards through the skin – this is known as vertical growth. The lesion presents as a nodule (lump) that has been rapidly enlarging over the previous weeks to months. It can arise de novo in normal-appearing skin, or within an existing melanoma of another type.
Nodular melanoma can penetrate deep within the skin within a few months of its first appearance.
Who gets nodular melanoma?
Nodular melanoma accounts for about 15% of all melanoma cases. Although more common in very fair skin (skin phototype 1 and 2), it may also occur in those who tan quite easily (phototype 3), and occasionally in brown or black skin (phototype 4-6).
Nodular melanoma is more common in males than in females. Most are over the age of 50 when it is diagnosed.
The main risk factors for nodular melanoma are:
What does nodular melanoma look like?
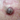
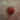
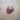
Nodular melanoma may arise on any site but is most common on exposed areas of the head and neck.
Nodular melanoma presents as a rapidly enlarging lump (over several weeks to months). The characteristics of nodular melanoma include:
Nodular melanoma can penetrate deep within the skin within a few months of its first appearance.
Who gets nodular melanoma?
Nodular melanoma accounts for about 15% of all melanoma cases. Although more common in very fair skin (skin phototype 1 and 2), it may also occur in those who tan quite easily (phototype 3), and occasionally in brown or black skin (phototype 4-6).
Nodular melanoma is more common in males than in females. Most are over the age of 50 when it is diagnosed.
The main risk factors for nodular melanoma are:
- Increasing age
- Previous invasive melanoma or melanoma in situ
- Many melanocytic naevi (moles)
- Multiple (>5) atypical naevi (funny-looking moles)
- Fair skin that burns easily
- It is less strongly associated with sun exposure than superficial spreading and lentigo maligna types of melanoma.
What does nodular melanoma look like?
Nodular melanoma may arise on any site but is most common on exposed areas of the head and neck.
Nodular melanoma presents as a rapidly enlarging lump (over several weeks to months). The characteristics of nodular melanoma include:
- Larger size than most moles >6 mm and often a centimetre or more in diameter at diagnosis
- Dome-shaped, often symmetrical firm lump
- Single colour or variable pigmentation – most often black, red or skin coloured
- Smooth, rough, crusted or warty surface
- Ulceration or bleeding
- Itching or stinging
- One-third of nodular melanomas are not pigmented. They lack the ABCDE criteria melanoma warning signs. (Asymmetry, Border irregularity, Colour variation, large Diameter).



What is the cause of nodular melanoma?
Nodular melanoma is due to the development of malignant pigment cells (melanocytes) along with the basal layer of the epidermis. These cells may occasionally arise from an existing melanocytic naevus (about 3%) but commonly occur within another type of melanoma or in previously normal-appearing skin. What triggers the melanocytes to become malignant is unknown, but it is likely to be a series of changes to the DNA. NRAS mutations are often found in patients with nodular melanomas.
What is the treatment for nodular melanoma?
The initial treatment of primary melanoma is to cut it out; the lesion should be completely excised with a 2-3 cm margin of normal tissue. Further treatment depends mainly on the Breslow thickness of the lesion.
What happens at follow-up of melanoma?
The primary purpose of follow-up is to detect recurrences early, but it also offers an opportunity to diagnose a new primary melanoma at the first possible opportunity. A second invasive melanoma occurs in 5-10% patients; an unrelated melanoma in situ affects in more than 20% of melanoma patients.
Follow-up appointments may include:
Tests are not typically worthwhile for stage 1/2 melanoma patients unless there are signs or symptoms of disease recurrence or metastasis. And no tests are thought necessary for healthy patients who have remained well for five years or longer after removal of their melanoma, whatever stage.
Nodular melanoma is due to the development of malignant pigment cells (melanocytes) along with the basal layer of the epidermis. These cells may occasionally arise from an existing melanocytic naevus (about 3%) but commonly occur within another type of melanoma or in previously normal-appearing skin. What triggers the melanocytes to become malignant is unknown, but it is likely to be a series of changes to the DNA. NRAS mutations are often found in patients with nodular melanomas.
What is the treatment for nodular melanoma?
The initial treatment of primary melanoma is to cut it out; the lesion should be completely excised with a 2-3 cm margin of normal tissue. Further treatment depends mainly on the Breslow thickness of the lesion.
What happens at follow-up of melanoma?
The primary purpose of follow-up is to detect recurrences early, but it also offers an opportunity to diagnose a new primary melanoma at the first possible opportunity. A second invasive melanoma occurs in 5-10% patients; an unrelated melanoma in situ affects in more than 20% of melanoma patients.
- Self-skin examination
- Routine skin checks by a patient's preferred health professional
- Follow-up intervals are preferably six-monthly for five years for patients with stage 1 disease, three-monthly or four-monthly for five years for patients with stage 2 or 3 disease, and yearly after that for all patients.
- Individual patient’s needs should be considered before an appropriate follow-up is offered
- Provide education and support to help the patient adjust to their illness
Follow-up appointments may include:
- A check of the scar where the primary melanoma was removed
- A feel for the regional lymph nodes
- A general skin examination
- A full physical examination
- In those with many moles or atypical moles, baseline whole-body imaging and sequential macro and dermoscopic images of melanocytic lesions of concern (mole mapping).
- Blood tests, including LDH
- Imaging: ultrasound, X-ray, CT, MRI and PET scan.
Tests are not typically worthwhile for stage 1/2 melanoma patients unless there are signs or symptoms of disease recurrence or metastasis. And no tests are thought necessary for healthy patients who have remained well for five years or longer after removal of their melanoma, whatever stage.

List of literature
- Lomas A., Leonardi-Bee J., Bath-Hextall F. A systematic review of worldwide incidence of nonmelanoma skin cancer. Br J Dermatol 2012; 166: 1069–80.
- Karjalainen S1, Salo H., Teppo L. Basal cell and squamous cell carcinoma of the skin in Finland. Site distribution and patientsurvival. Int J Dermatol. 1989 Sep; 28(7): 445–50.
- Bastiaens MT, Hoefnagel JJ, Bruijn JA et al. Differences in age, site distribution, and sex between nodular and superficial basal cell carcinoma indicate different types of tumors. J Invest Dermatol 1998; 110:880–4.
- Luz FB, Ferron C., Cardoso GP. Surgical treatment of basal cell carcinoma: an algorithm based on the literature. An Bras Dermatol. 2015 May-Jun; 90(3): 377–83.
- Julien Lanoue, Gary Goldenberg. Basal Cell Carcinoma, А Comprehensive Review of Existing and Emerging Nonsurgical Therapies. J Clin Aesthet Dermatol. 2016 May; 9 (5): 26–36.]
- Vijlder, H., Sterenborg, H., Neumann, H., Robinson, D., Haas, E. (2012). Light Fractionation Significantly Improves the Response of Superficial Basal Cell Carcinoma to Aminolaevulinic Acid Photodynamic Therapy: Five-year Follow-up of a Randomized, Prospective Trial. Acta Dermato Venereologica, 92 (6), 641–647. doi: 10.2340/00015555-1448
- Lehmann, P. (2007). Methyl aminolaevulinate?photodynamic therapy: a review of clinical trials in the treatment of actinic keratoses and nonmelanoma skin cancer. British Journal of Dermatology, 156(5), 793–801. doi: 10.1111/j.1365-2133.2007.07833.x.
- Ceilley RI, Del Rosso JQ. Current modalities and new advances in the treatment of basal cell carcinoma. Int J Dermatol. 2006 May; 45(5): 489–98.
- Wysong, A., Aasi, S. Z., Tang, J. Y. (2013). Update on Metastatic Basal Cell Carcinoma: A Summary of Published Cases From 1981 Through 2011. JAMA Dermatology, 149(5), 615.
- Sekulic A, Migden MR, Basset-Seguin N., Garbe C., Gesierich A., Lao CD., Miller C., Mortier L., Murrell DF., Hamid O., Quevedo JF., Hou J., McKenna E., Dimier N., Williams S., Schadendorf D., Hauschild A.; ERIVANCE BCC Investigators.Long-term safety and efficacy of vismodegib in patients with advanced basal cell carcinoma: finalupdate of the pivotal ERIVANCE BCC study. BMC Cancer. 2017 May 16; 17(1):3 32. doi: 10.1186/s12885-017-3286-5.
- Lear JT., Migden MR., Lewis KD., Chang ALS., Guminski A., Gutzmer R., Dirix L., Combemale P., Stratigos A., Plummer R., Castro H, Yi T., Mone M., Zhou J., Trefzer U., Kaatz M., Loquai C., Kudchadkar R., Sellami D., Dummer R. Long-term efficacy and safety of sonidegib in patients with locally advanced and metastatic basal cell carcinoma: 30-month analysis of the randomized phase 2 BOLT study.J Eur Acad Dermatol Venereol. 2018 Mar; 32 (3): 372–381. doi: 10.1111/jdv.14542. Epub 2017 Nov 6.
- Wieman TJ., Shively EH., Woodcock TM. Responsiveness of metastatic basal-cell carcinoma to chemotherapy. A case report. Cancer. N1983; 52 (9): 1583–1585.
- Coker DD, Elias EG, Viravathana T, et al. Chemotherapy for metastatic basal cell carcinoma. Arch Dermatol. 1983; 119 (1): 44–50.
- Guthrie TH., Jr, McElveen LJ., Porubsky ES., Harmon JD. Cisplatin and doxorubicin. An effective chemotherapy combination in the treatment of advanced basal cell and squamous carcinoma of the skin. Cancer. 1985; 55 (8): 1629–1632.
- Bason MM., Grant-Kels JM., Govil M. Metastatic basal cell carcinoma: response to chemotherapy. J Am Acad Dermatol. 1990; 22 (5 Pt 2): 905–908.
- Khandekar JD. Complete response of metastatic basal cell carcinoma to cisplatin chemotherapy: a report of two patients. Arch Dermatol. 1990; 126 (12): 1,660.
- Denic S. Preoperative treatment of advanced skin carcinoma with cisplatin and bleomycin. Am J Clin Oncol. 1999; 22 (1): 32–34.
- Jefford M., Kiffer JD., Somers G., et al. Metastatic basal cell carcinoma: rapid symptomatic response to cisplatin and paclitaxel. ANZ J Surg. 2004; 74 (8): 704–705.
- Moeholt K., Aagaard H., Pfeiffer P., Hansen O. Platinum-based cytotoxic therapy in basal cell carcinoma-a review of the literature. Acta Oncol. 1996; 35 (6): 677–682.
- Carneiro BA., Watkin WG., Mehta UK., Brockstein BE. Metastatic basal cell carcinoma: complete response to chemotherapy and associated pure red cell aplasia. Cancer Invest. 2006; 24 (4): 396–400.


